Last Updated on 1 week ago
Disclaimer:
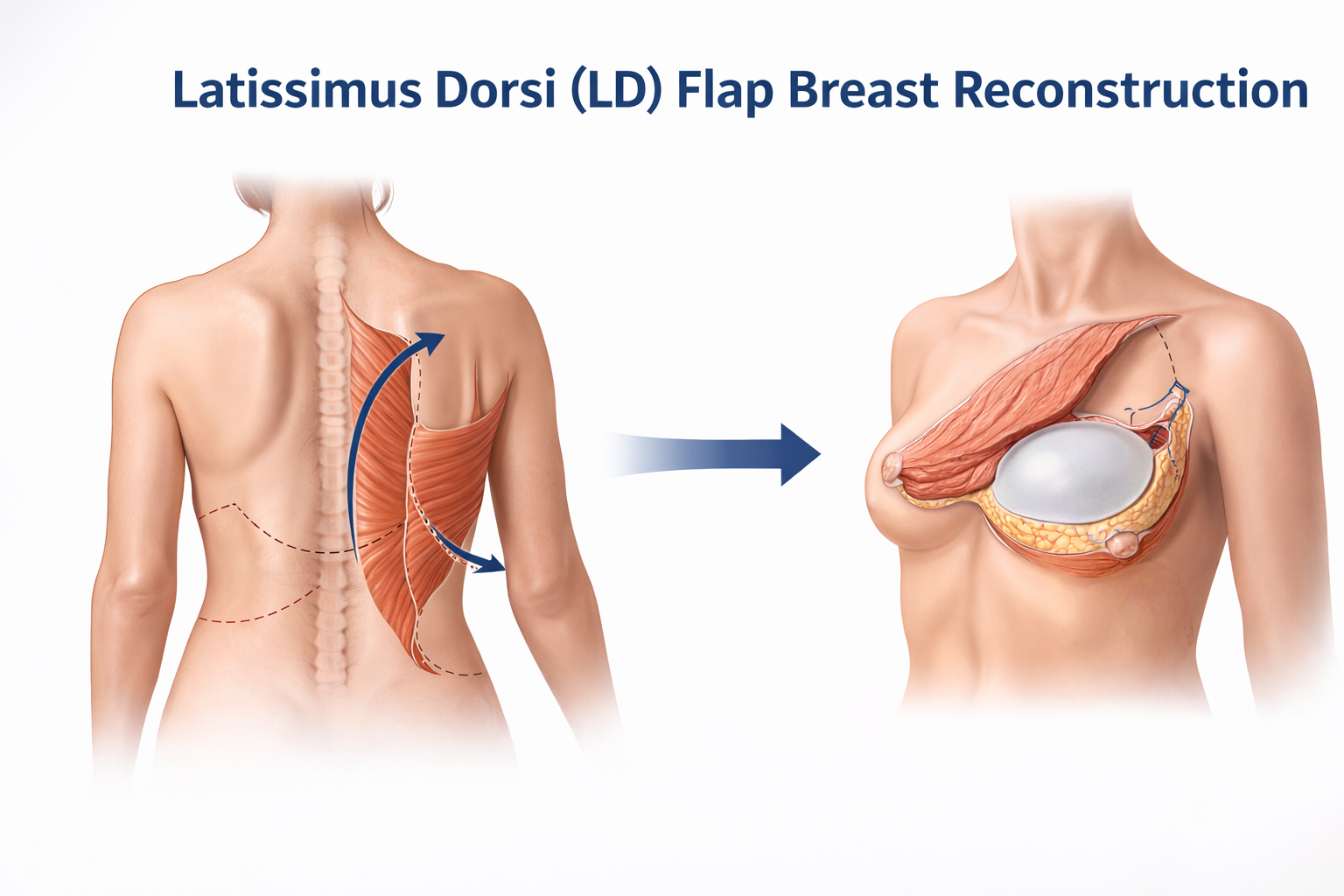
This article shares one individual patient’s personal experience with latissimus dorsi (LD) flap breast reconstruction. Every patient’s medical situation, anatomy, treatment plan, and outcomes are different. This content is provided for educational and informational purposes only and should not be considered medical advice.
BRA Society does not provide medical care, diagnosis, or treatment recommendations. Patients should consult with qualified medical professionals and seek multiple opinions when making decisions about breast reconstruction or any surgical procedure.
Some reconstruction options may involve the use of muscle while others may not. The most appropriate option depends on individual medical circumstances. We encourage patients to learn about all available options including options that don’t compromise the muscle (examples: DIEP, GAP, PAP, LAP, TDAP), and discuss risks and benefits with their care team.
A Diagnosis That Changed Everything
When I reflect on my initial diagnosis of triple-positive stage 3C inflammatory invasive breast cancer, it feels like it was a lifetime ago. Yet, I continue to live with the consequences of complications and regrets every day.The shock of receiving a cancer diagnosis makes the prospect of making life-altering decisions daunting, especially when there are no guarantees and numerous potential side effects, regardless of the chosen option.
The Most Important Lesson: Be Your Own Advocate
One of the most important lessons I’ve learned from my experience is the necessity of being your own advocate.
It’s essential to research your reconstruction options more thoroughly than just relying on what you’re told in the doctor’s office. Sometimes doctors may provide misinformation or misdiagnoses and expect you to accept their word without considering your own feelings or experiences.
Understanding the benefits and potential repercussions of any surgical procedure—especially breast reconstruction after mastectomy or lumpectomy—is critical. This includes researching possible complications and weighing those risks against other options, including choosing no reconstruction at all.
Why I Chose LD Flap Reconstruction
When I decided to undergo Latissimus Dorsi (LD) flap reconstruction, I was not in a good relationship. I had not researched the pros and cons of the procedure and feared the complexity of the surgery.
I was also concerned about the need to travel out of state for DIEP flap surgery. At the time, I didn’t fully understand the type of breast cancer I had, and I worried about how much recovery time each option would require.
My decisions were shaped by fear, timing, and incomplete information.
Trying Not to Burden Anyone
When I was diagnosed, my children were pre-teens, heavily involved in school activities and sports. My ex-husband, a scallop fisherman, was often away on two-week trips and home for only a week, if we were lucky.
I didn’t want to burden family or friends with driving my girls, helping around the house, taking me to appointments, or just lending a hand.
This journey taught me that accepting help is not weakness—it is survival.
The Power of Community Support
I was fortunate to have friends who proactively offered support. They gave my kids rides, picked up groceries, dropped off meals, took me to appointments and surgeries, and provided comfort when I needed to cry.
Even strangers showed me kindness I never expected.
One neighbor even took our dog to be euthanized after she was hit by a car while I was attending a cancer patient event. I could never have imagined someone doing that for me in such a devastating moment.
Because of this support, I worried less about how long recovery would take and focused more on surviving.

When My Reconstruction Plan Fell Apart
My original mastectomy was a skin-sparing procedure with immediate expanders placed. I felt disheartened—like a rock had been dropped on my chest—when I was told everything would need to be undone.
If I opted for radiation under those circumstances, it would eliminate my reconstructive options.
I don’t recall being clearly told that I had inflammatory breast cancer—or understanding that it involved the skin. Had I known, I never would have chosen skin-sparing surgery.
Feeling Backed Into a Corner
I felt trapped. I had to choose between starting over with new doctors and pursuing DIEP flap surgery, delaying treatment, or staying with my surgeon and choosing TRAM or LD flap reconstruction.
All of these options terrified me. LD reconstruction required the least recovery time, so I chose it.
What I thought might be a solution turned into false hope.
Severe Complications After LD Surgery
I developed a seroma, a pocket of fluid that grew larger each week. I endured six weeks of failed sclerotherapy, involving repeated needle injections, long appointments, compression wraps, and exhausting travel.
On the sixth visit, a cracked drain sent me back to the emergency room. Even then, the treatment failed.
Eventually, the seroma calcified, forming a hardened capsule that required additional surgery.
Risks I Wasn’t Truly Informed About
I vaguely recall being told about “possible” side effects—but not how likely they were.
According to published research:
- 95% of patients develop seromas
- 15% develop hypertrophic scarring
- 15% require additional surgery for hematomas
- 10% suffer from chronic back pain
I don’t remember being told these odds clearly—or at all.
Living With Permanent Physical Damage
As a result of LD reconstruction and corrective surgeries, I now live with nerve damage, limited shoulder range of motion, muscle weakness, chronic pain, and regular rib dislocations.
I can’t lift, twist, or move the way I used to. I can’t reach the top shelf anymore.
Sometimes coughing or sneezing dislocates my ribs. Other times I feel sudden, stabbing nerve pain under my arm.
To someone looking at me, I may appear fine—but many cancer-related injuries are invisible.

Medical Dismissal Nearly Cost Me My Life
During chemotherapy, I developed Bell’s palsy and a blood clot. A doctor nearly sent me home without imaging.
If I had trusted that assessment, I likely wouldn’t be alive today.
Earlier imaging dismissed my concerns as fibrocystic, even though follow-up was recommended and never communicated. My primary care office also failed to ask why I hadn’t followed up for over a year.
Doctors protect themselves. Patients must protect themselves too.
Reconstruction, Abuse, and Body Image
My primary fear about reconstruction was simple: I wasn’t emotionally ready to be flat.
I was in a deeply unhealthy marriage. On the morning of my third chemotherapy treatment, my husband left without saying goodbye. When I confronted him, he told me:
“You deserve cancer.”
That moment changed everything.
Domestic Violence and Further Trauma
After reconstruction and divorce, I entered another relationship that eventually became violent.
When he insulted my body—specifically my lack of nipples—I finally told him to leave.
My mental health and body image were beyond damaged.
I later obtained a Protection from Abuse order after continued harassment.
Implant Rupture and Breast Implant Illness
Years later, doctors discovered a slow implant rupture, likely linked to prior assault.
I began experiencing symptoms consistent with breast implant illness, including fatigue, joint and muscle pain, brain fog, anxiety, depression, sleep issues, and GI problems.
My body was telling me something was wrong.
Fighting for Implant Removal
Despite agreeing to removal, my surgeon’s office delayed my surgery for months and blamed insurance.
After contacting my insurer directly, I learned the truth: the office hadn’t submitted my paperwork until the day I called.
Approval came quickly—but they delayed telling me.
Choosing Myself
I ultimately had my implants removed.
I am still living with the permanent effects of LD reconstruction—but removing the implants felt like reclaiming my body.
By then, I was married to a man who treats me with unconditional love. When I asked if my breast “looked weird,” he said:
“There is no right answer. I love you exactly as you are.”
Why I Share This Story
Cancer takes so much from us.
It should never take away our right to change our minds.
If I had been better informed—about inflammatory breast cancer, reconstruction risks, and implant illness—I may have made different decisions.
If there is one lesson I’ve taken away, it’s this: be your own advocate. Bring someone you trust. Ask hard questions. And remember—no one should ever have to face this journey alone.
Chronological Sequence of Events
- September 20, 2013 — Received stage 3C invasive ductal carcinoma diagnosis
- October 2013 — Began four rounds AC chemo, followed by 12 rounds Taxol with Herceptin for one year
- December 16, 2013 — Woke up with swollen face/neck; subsequent blood clot
- January 2014 — Derogatory comment by ex-husband
- April 3, 2014 — Last Taxol dose / end of chemotherapy
- May 2, 2014 — Bilateral mastectomy with expanders placed
- July 7, 2014 — Removal of left expander
- July 31, 2014 — Began 30 rounds of radiation with alternating bolus
- September 11, 2014 — Completed radiation with 3rd and 4th degree burns
- October 2014 — Tubal ligation
- November 2014 — Developed Bell’s palsy
- March 25, 2015 — LD flap reconstruction
- June 2015 — Developed seroma; six weeks of failed sclerotherapy
- July–September 2015 — Seroma removal and corrective surgeries
- October 18, 2021 — Domestic assault
- April 26, 2022 — Protection from Abuse order approved
- September 28, 2022 — Remarried
- September 2023 — Incidental finding of ruptured implant
- October 2023 — Implant replacement surgery
- January 2024 — Final decision for implant removal
- March 2024 — Insurance approval obtained after escalation
- May 8, 2024 — Implant removal surgery
References and Resources
- Seroma: https://en.wikipedia.org/wiki/Seroma
- Sclerotherapy: https://en.wikipedia.org/wiki/Sclerotherapy
- Hypertrophic scar: https://en.wikipedia.org/wiki/Hypertrophic_scar
Burgic M, et al. Complications following autologous latissimus flap breast reconstruction. Bosn J Basic Med Sci. 2010.
Ten Years of Remission, One Woman’s Cancer Story, Midcoast Villager
BreastCancer.org — Breast Implant Illness (BII)
Lincoln County Television, American Cancer Society Making Strides Walk, October 2024

No comment